New front in war on Alzheimer’s, other protein-folding diseases
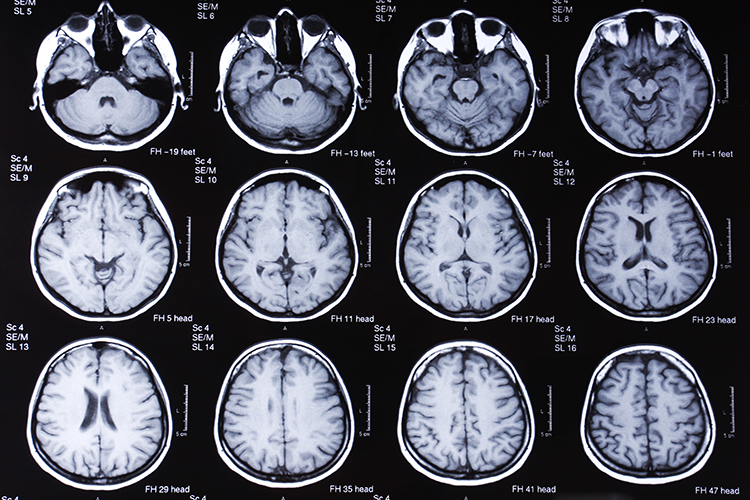
Many neurodegenerative diseases, including Alzheimer's, have been linked to the accumulation of improperly folded proteins in the brain. How they collect is a mystery, but Andrew Dillin and his lab have found a new mechanism cells use to prevent misfolding that could lead to new types of therapies for these diseases.
October 16, 2014
A surprise discovery that overturns decades of thinking about how the body fixes proteins that come unraveled greatly expands opportunities for therapies to prevent diseases such as Alzheimer’s and Parkinson’s, which have been linked to the accumulation of improperly folded proteins in the brain.
“This finding provides a whole other outlook on protein-folding diseases; a new way to go after them,” said Andrew Dillin, the Thomas and Stacey Siebel Distinguished Chair of Stem Cell Research in the Department of Molecular and Cell Biology and Howard Hughes Medical Institute investigator at the University of California, Berkeley.

A cell suffering heat shock is like a country besieged, where attackers first sever lines of communications. The pat-10 gene helps repair communication to allow chaperones to treat misfolded proteins. (Andrew Dillin graphic)
Dillin, UC Berkeley postdoctoral fellows Nathan A. Baird and Peter M. Douglas and their colleagues at the University of Michigan, The Scripps Research Institute and Genentech Inc., will publish their results in the Oct. 17 issue of the journal Science.
Cells put a lot of effort into preventing proteins – which are like a string of beads arranged in a precise three-dimensional shape – from unraveling, since a protein’s activity as an enzyme or structural component depends on being properly shaped and folded. There are at least 350 separate molecular chaperones constantly patrolling the cell to refold misfolded proteins. Heat is one of the major threats to proteins, as can be demonstrated when frying an egg – the clear white albumen turns opaque as the proteins unfold and then tangle like spaghetti.
Heat shock
For 35 years, researchers have worked under the assumption that when cells undergo heat shock, as with a fever, they produce a protein that triggers a cascade of events that field even more chaperones to refold unraveling proteins that could kill the cell. The protein, HSF-1 (heat shock factor-1), does this by binding to promoters upstream of the 350-plus chaperone genes, upping the genes’ activity and launching the army of chaperones, which originally were called “heat shock proteins.”
Injecting animals with HSF-1 has been shown not only to increase their tolerance of heat stress, but to increase lifespan.
Because an accumulation of misfolded proteins has been implicated in aging and in neurodegenerative diseases such as Alzheimer’s, Parkinson’s and Huntington’s diseases, scientists have sought ways to artificially boost HSF-1 in order to reduce the protein plaques and tangles that eventually kill brain cells. To date, such boosters have extended lifespan in lab animals, including mice, but greatly increased the incidence of cancer.
Dillin’s team found in experiments on the nematode worm C. elegans that HSF-1 does a whole lot more than trigger release of chaperones. An equal if not more important function is to stabilize the cell’s cytoskeleton, which is the highway that transports essential supplies – healing chaperones included – around the cell.
“We are suggesting that, rather than making more of HSF-1 to prevent diseases like Huntington’s, we should be looking for ways to make the actin cytoskeleton better,” Dillin said. Such tactics might avoid the carcinogenic side effects of upping HSF-1.
Dillin is codirector of the Paul F. Glenn Center for Aging Research, a new collaboration between UC Berkeley and UC San Francisco supported by the Glenn Foundation for Medical Research. Center investigators will study the many ways that proteins malfunction within cells, ideally paving the way for novel treatments for neurodegenerative diseases.
A cell at war
Dillin compares a cell experiencing heat shock to a country under attack. In a war, an aggressor first cuts off all communications, such as roads, train and bridges, which prevents the doctors from treating the wounded. Similarly, heat shock disrupts the cytoskeletal highway, preventing the chaperone “doctors” from reaching the patients, the misfolded proteins.

Chaperones help newborn proteins (polypeptides) fold properly, but also fix misfolded proteins.
“We think HSF-1 not only makes more chaperones, more doctors, but also insures that the roadways stay intact to keep everything functional and make sure the chaperones can get to the sick and wounded warriors,” he said.
The researchers found specifically that HSF-1 up-regulates another gene, pat-10, that produces a protein that stabilizes actin, the building blocks of the cytoskeleton.
By boosting pat-10 activity, they were able to cure worms that had been altered to express the Huntington’s disease gene, and also extend the lifespan of normal worms.
Dillin suspects that HSF-1’s main function is, in fact, to protect the actin cytoskeleton. He and his team mutated HSF-1 so that it no longer boosted chaperones, demonstrating, he said, that “you can survive heat shock with the normal level of heat shock proteins, as long as you make your cytoskeleton work better.”
He noted that the team’s results – that boosting chaperones is not essential to surviving heat stress – were so contradictory to current thinking that “I made my post-docs’ lives hell for three years” insisting on more experiments to rule out errors. Yet, when Dillin presented the results recently to members of the protein-folding community, he said the first reaction of many was, “That makes perfect sense.”
Dillin’s colleagues include Milos S. Simic and Suzanne C. Wolff of UC Berkeley, Ana R. Grant of the University of Michigan in Ann Arbor, James J. Moresco and John R. Yates III of Scripps in La Jolla, Calif., and Gerard Manning of Genentech, South San Francisco, Calif. The work is funded by the Howard Hughes Medical Institute as well as by the National Institute of General Medical Sciences (8 P41 GM103533-17) and National Institute on Aging (R01AG027463-04) of the National Institutes of Health.
RELATED INFORMATION