$47 million grant to explore how a healthy lifestyle changes the aging brain
Study will be the first large-scale investigation of how lifestyle interventions affect biological markers of Alzheimer’s dementia in the brain
July 29, 2019
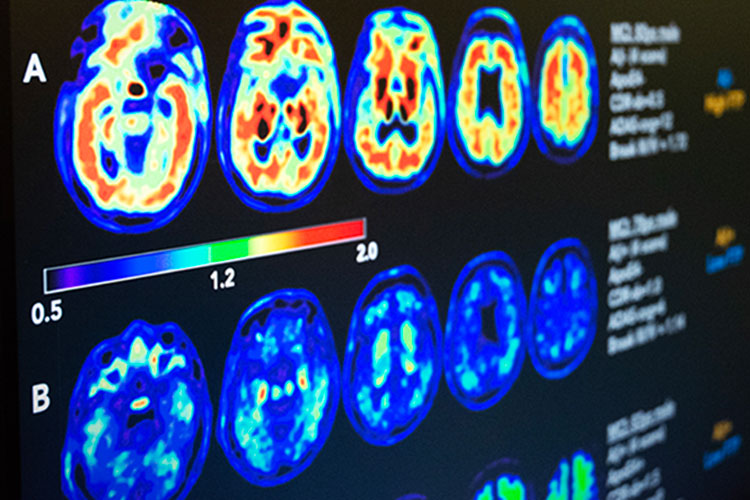
The new funding will add positron emission tomography (PET) and magnetic resonance imaging (MRI) to the upcoming U.S. POINTER study, which will explore how lifestyle changes affect memory and thinking in older adults. (UC Berkeley photo by Malachi Tran)
UC Berkeley was awarded a five-year grant expected to total $47 million from the U.S. National Institute on Aging (NIA) to incorporate advanced brain imaging into an Alzheimer’s Association-led study to explore whether lifestyle changes can protect memory in those at risk of developing dementia.
The expanded study will be the first large-scale investigation of how lifestyle interventions, which include exercise, diet, cognitive stimulation and health coaching, affect well-known biological markers of Alzheimer’s and dementia in the brain.
“A healthy diet and lifestyle are generally recognized as good for health, but this study is the first large randomized controlled trial to look at whether lifestyle changes actually influence Alzheimer’s disease-related brain changes,” said Susan Landau, a research neuroscientist at Berkeley’s Helen Wills Neuroscience Institute, and principal investigator of the add-on study.
The U.S. study to Protect brain health through lifestyle Intervention to Reduce risk (U.S. POINTER) is a two-year, $35 million Alzheimer’s Association-sponsored multisite clinical trial designed to test whether healthy diet, physical activity, and social and intellectual challenge can protect thinking and memory in older adults.
The new award of $47 million from the NIA, part of the U.S. National Institutes of Health, (NIH grant number R01AG062689) will support the U.S. POINTER Neuroimaging Ancillary Study, which will use advanced brain imaging techniques to assess how these lifestyle modifications can affect brain health.
As part of the ancillary study, researchers will use magnetic resonance imaging (MRI) to monitor participants’ overall and regional brain shape, size and blood flow, and indicators of vascular disease that impacts the brain. It will also use positron emission tomography (PET) to track the presence of beta-amyloid and tau proteins in the brain.
Build up of beta-amyloid and tau proteins occur in Alzheimer’s dementia and are linked to memory decline that occurs as the disease progresses. These biological markers are also now considered essential in large-scale, late-stage therapy trials in Alzheimer’s.
“The U.S. POINTER study gives us an opportunity to ask whether diet and exercise can actually change the brain, and ultimately the risk of Alzheimer’s disease and other dementias,” Landau said. “We also plan to study whether these markers, when measured at the beginning of the study, can predict who will respond best to the intervention, which could inform future precision-medicine approaches to healthcare.”

Susan Landau, a research neuroscientist at UC Berkeley’s Helen Wills Neuroscience Institute, is principal investigator of the add-on study. (UC Berkeley photo by Malachi Tran)
According to the Alzheimer’s Association 2019 Alzheimer’s Disease Facts and Figures report, an estimated 5.8 million Americans of all ages are living with Alzheimer’s dementia, and Alzheimer’s is the sixth-leading cause of death in the U.S. Barring the development of medical breakthroughs, the number may nearly triple to 13.8 million by 2050.
Previous results suggest that lifestyle changes may benefit the brain health of older adults more than pharmacological treatments. For example, the Finnish Geriatric Intervention Study to Prevent Cognitive Impairment and Disability (FINGER) showed that in at-risk adults, lifestyle intervention improved cognitive function by 25 percent relative to adults who only received health education.
U.S. POINTER is unique in its recruitment approach, which specifically aims to include a geographically and racially diverse population. This can help ensure the intervention will be applicable to a large proportion of older individuals. Four sites (Winston-Salem, NC; Houston, TX; Davis, CA, and Chicago, IL) have been chosen for U.S. POINTER, with one more site planning to come online later this year.
The study hopes to recruit around 2,000 participants, just over one-half of which will be assessed with PET imaging at the start of the study and at two years to measure the build up of amyloid and tau. They will also be assessed with MRI at baseline, one year, and two years to measure the size of brain regions, identify lesions related to strokes or other vascular changes, and observe changes in brain blood flow.
“This groundbreaking project is an unparalleled examination of how lifestyle ‘therapies’ may change our brain in ways that are related to Alzheimer’s disease, vascular dementia and overall brain health,” said Maria C. Carrillo, Ph.D., Chief Science Officer of the Alzheimer’s Association.
“U.S. POINTER is designed to determine what lifestyle interventions have a tangible impact on our brains. The addition of brain imaging is an important component that could provide the roadmap for brain health to reduce the risk of dementia before symptoms have a chance to appear,” Carrillo said.
RELATED INFORMATION